‘Spleen-on-a-chip’ opens the way for understanding sickle cell disease better
Chip mimics human spleen functions and simulates disease mechanisms
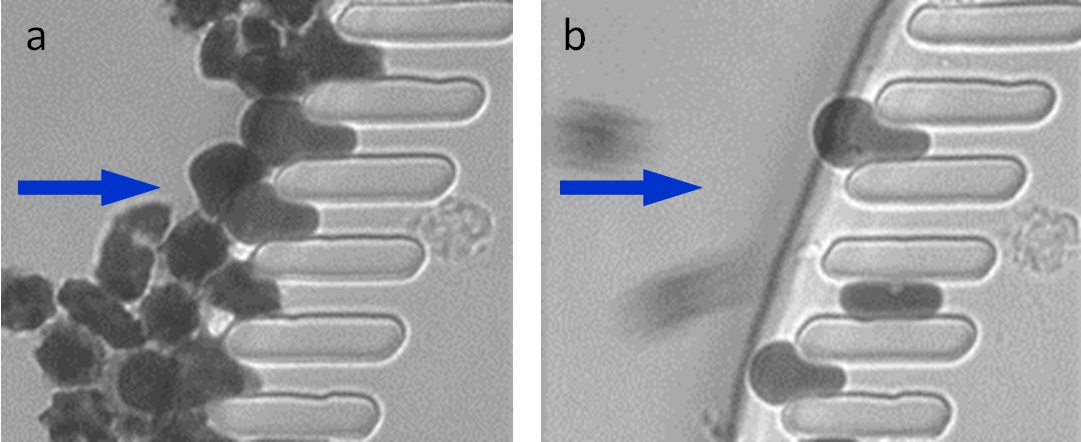
When oxygen levels are low, sickled red blood cells tend to clog the microslits in the spleen-on-a-chip as they move from left to right (a). But once oxygen levels are higher, the cells unsickle and can pass through (b). (Credit: Courtesy of the researchers)
The body’s spleen plays a vital role in filtering and removing old and damaged red blood cells. But sickle cell disease, which afflicts about 120 million people globally, can impair the organ’s functions and, in some cases, lead to death, especially in infants.
Now, scientists have developed a “spleen-on-a-chip” which aims to investigate the spleen’s filtration function in physiology and disease. They also believe that, in the future, the chip, which mimics the spleen’s functions in the body, can be used to better understand related disease pathology, study the efficacy of drugs or treatments for life-threatening spleen ailments, and help patients keep tabs on their condition.
The findings on the development of the spleen-on-a-chip were published online in The Proceedings of the National Academy of Sciences journal in February 2023.
Clogged spleens
The thumb-drive-sized chip is a “microfluidic” device made of a clear and flexible polymer formed into channels that contain human cells. It simulates conditions in the human body, such as the speed at which blood flows and the oxygen levels in the spleen.
The device has two modules. The first is the “S chip” module, which mimics the function of tiny gaps or microslits between cells that form walls of a part of the spleen that filters blood.
Normally, red blood cells, which are more than five times thinner than a strand of hair, can easily change their shape to squeeze through the spleen’s microslits. But in sickle cell disease, red blood cells are stiffened and distorted into a sickle shape under low oxygen levels. These stiff cells have difficulty changing their shape to pass through the microslits easily, which blocks the slits and causes red blood cells to be trapped in the spleen.
When there is severe clogging of sickled red blood cells, it can lead to a splenic sequestration crisis as many blood cells get stuck in the spleen. This leads to a person becoming very anaemic due to a lack of red blood cells circulating in the body. In some children with sickle cell disease, it can result in death within hours.
With the S chip module, the scientists found that at low oxygen levels, sickled cells could not pass through the device’s microslits due to their stiffness. When they raised the chip’s oxygen levels, the clog cleared as the blood cells unsickled and passed through the slits.
Slow clearing of blockage
The second spleen-on-a-chip module is the “M chip”, which models the behaviour of immune cells called macrophages in the spleen. Macrophages remove diseased or damaged red blood cells, as well as those that are stiff or cannot change their shape to pass through the microslits. They do so by “eating” and then destroying these cells.
The scientists found that at low oxygen levels, when sickled cells cause severe blockage, the macrophages took a long time to digest stiff sickled red blood cells, slowing the clearing of the clog. However, raising oxygen levels allowed the sickled cells to unsickle, which let the macrophages digest them normally and clear the blockage faster.
The findings demonstrate the importance of a homeostatic balance between retaining red blood cells and eliminating trapped red blood cells by macrophages in the spleen. Following up on their findings, the researchers are studying the behaviour of cells in the spleen-on-a-chip to assess the efficacy of drugs used to treat sickle cell disease.
The research team was led by Professor Subra Suresh, Vannevar Bush Professor Emeritus and former Dean of Engineering at Massachusetts Institute of Technology (MIT), and former President of Nanyang Technological University, Singapore (NTU Singapore); Professor Ming Dao, MIT Principal Research Scientist and NTU Visiting Professor; and Professor Pierre Buffet, Medical Director of France’s Institut Pasteur and Professor of Cell Biology at Université Paris Cité.
Others involved include Dr Fang Kong, a research fellow from NTU’s School of Biological Sciences, and Dr Fuyin Zheng, a research fellow at the school during the time of the study.
The study was funded by NTU Singapore and the United States’ National Institutes of Health.
Details of the research can be found in “Microfluidic study of retention and elimination of abnormal red blood cells by human spleen with implications for sickle cell disease” in The Proceedings of the National Academy of Sciences (2023).

-and-dr-dorrain-low-from-ntu-singapore's-lkcmedicine.tmb-listing.jpg?Culture=en&sfvrsn=b389b500_1)
.tmb-listing.jpg?Culture=en&sfvrsn=82921582_1)

.tmb-listing.jpg?Culture=en&sfvrsn=ba129532_1)